Table Of Contents
- What Are the Factors Contributing to Prostate Gland Enlargement?
- What Are the Factors Contributing to Prostate Gland Enlargement?
- What Are the Symptoms of Prostate Gland Enlargement?
- What Are the Risk Factors for Prostate Gland Enlargement?
- Can Prostate Gland Enlargement Be Cured?
- What Are Some of the Preventive Measures?
Have you heard of prostate gland enlargement? Perhaps you have heard it from someone casually or in the movies. But what does an enlarged prostate gland mean? The men need to give special attention to this term, as they may experience this condition at some point.
Since you are here to learn a little more about prostate gland enlargement, we have explained everything in this article. Read on to find out.
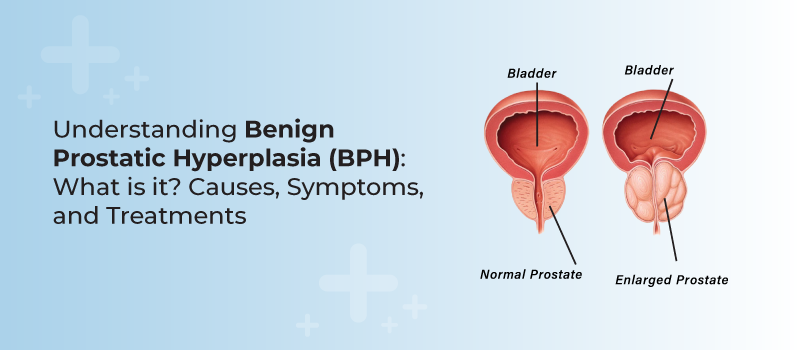
What is Prostate Gland Enlargement?
Let’s begin with what prostate gland enlargement is. So, it is also known as benign prostatic hyperplasia. It is now a common condition, so you need not worry about it. It’s quite common in aging men.
As men get older, their prostate gland goes through several changes. It could lead to a variety of complications and symptoms.
Age has an impact on both women and men, so you need not get anxious. However, it is essential to detect it a little early so that you can lead a stress-free life.
What Are the Factors Contributing to Prostate Gland Enlargement?
First, it’s the hormonal changes. When men start aging, the balance of the hormones in their bodies will also change. The hormonal fluctuation is fairly normal, and it could lead to the growth of the prostate gland.
Second, it could be cellular growth. The prostate gland has many smaller glands as well as smooth muscle tissue. When men start aging, the cells will also go through several changes. This leads to cellular growth and hyperplasia.
Third, it could also be chronic inflammation. The prostate gland may be inflamed, which is also known as prostatitis. It is quite common in older men.If the inflammation is persistent, the prostate gland will become large, and there will be other symptoms too.
Now that you know the prostate gland enlargement causes, let’s move on to the symptoms. How else would you know that you have prostate gland enlargement?
What Are the Symptoms of Prostate Gland Enlargement?
Prostate gland enlargement has several symptoms:
- Frequent Urination: Men who have this condition will need to urinate quite often. They feel the need to urinate many times at night. This may disrupt their sleep and affect their sex life too.
- Trouble starting urination: So, having this BPH condition could cause issues with starting urination. Men may feel pressured or strained to do so.
- Weak urine stream: Men with BPH will feel their urine stream is not exactly consistent. It may be weak. For example, it may start and stop. Don’t be alarmed! It is one of the symptoms of BPH.
- Bladder not emptying: BPH could lead to incomplete emptying of the bladder. This could cause some discomfort.
- Urinary tract infection: Urinary tract infection is also one of the symptoms that may cause itching, a foul smell, a burning sensation, and other problems.
Prostate gland enlargement symptoms should not be ignored. You need to see a doctor immediately.
What Are the Risk Factors for Prostate Gland Enlargement?
<class=”chro_data”>There are a few risk factors for prostate gland enlargement that you should be aware of:
1. Age factor:
As we told you earlier, aging men are more prone to BPH. The risk increases with age, particularly after age 50. Check out the prostate size chart by age and find out whether yours is normal or not.
2. Family history:
Men who have a family history of BPH or prostate cancer may have a higher risk of getting this condition
3.Lifestyle:
Maybe you are lazy or are too heavy. Maybe you are a smoker and an alcoholic. All these are risk factors.
Can Prostate Gland Enlargement Be Cured?
Yes! There is a cure for enlarged prostate gland. There are different treatment options for you.
First, the healthcare provider may ask you to wait. They want you to monitor the condition over a period of time before sharing their thoughts on the best treatment.
Next comes medication. There are many medications that are available to treat this condition. This may also include alpha-blockers or some form of inhibitor. These will help shrink the prostate gland.
Third, the doctor may suggest a minimally invasive process. This is best for those who have moderate-to-severe BPH. If medications are not working for you, this is the best option.
Fourth, there is surgical intervention too. Speak to the specialist about the procedure. This may involve the removal of the prostate gland or just a part of it.
Fifth, there is surgical intervention. This is an invasive procedure, and it is best for those who have severe BPH.
What Are Some of the Preventive Measures?
We are sure you are now aware of the basic facts about an enlarged prostate. But don’t worry; we can share some preventive measures too.
First, you should be active and maintain a healthy life. Exercise regularly, maintain a healthy weight, and start eating a balanced diet. Include all kinds of fruits and veggies.
Second, you should go for regular health checks. Men who are nearing their 50s should do this for sure, especially if there is a family history of BPH.
Third, it would be a good idea to manage health conditions such as diabetes and hypertension. Maintain a healthy weight and take better care of your heart.
Summing Up
It looks like you are now aware of what prostate gland enlargement is and how it affects men after the age of 50. You are aware of the factors, symptoms, and possible treatment options.
There are many medical advancements now, so you need not worry. If you have an enlarged prostate gland, go see a specialist today and take their expert advice.
Frequently Asked Questions
1. What happens to the prostate gland as a result of ageing?
Ans.The prostate gets enlarged once men cross the age of 50. But, this also depends on the lifestyle and family history of the man.
2. Can an enlarged prostate go back to normal?
Ans. Yes! There are medications, minimally invasive procedures, and invasive procedures to shrink the size of the enlarged prostate.
3. What is the fastest way to shrink an enlarged prostate naturally?
Ans. The best remedy for prostate gland enlargement is an improved lifestyle. Though this can only help manage the situation. If the condition is not serious, then medications will be a quick way to shrink the enlarged prostate.
4. Can you live a long life with an enlarged prostate?
Ans. It’s not cancer, so you will live a long life as long as you are healthy and free from any diseases.