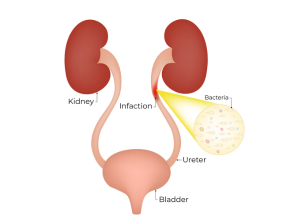
Recurrent Urinary Tract Infections (UTIs)
Recurrent urinary tract infections refer to repeated episodes of infection affecting the bladder or urinary tract over a period of time. Doctors typically define it as two or more UTIs within six months, or three or more within a year.
These infections may feel similar to a typical UTI, but their repeated nature can significantly affect daily comfort, emotional wellbeing, and overall quality of life. For some individuals, the pattern is linked to anatomical or medical factors, while for others, triggers such as sexual activity, hormonal changes, or bladder habits play a major role.
Understanding the underlying cause is essential to choosing the right treatment plan and preventing future episodes.
Symptoms of Recurrent Urinary Tract Infections
Symptoms of recurrent UTIs are the same as a regular bladder infection, but the frequency and persistence can make them more distressing. Many people experience cycles of flare-ups followed by symptom-free periods.
Common symptoms include:
- Frequent episodes of burning or painful urination
- Recurring urgency and frequency of urination
- Lower abdominal or pelvic pain during flare-ups
- Cloudy, dark, or occasionally bloody urine
- Strong or foul-smelling urine
- Feeling like the bladder doesn’t empty fully
- Low-grade fever during active episodes
- Frequent nighttime urination (nocturia)
- Persistent pelvic discomfort even between infections
- Fatigue and reduced quality of life
- Anxiety or worry about when the next infection will occur
- Symptoms occurring after sexual intercourse, especially in women prone to post-coital UTIs
Because these infections recur, even mild symptoms can be concerning and emotionally draining for patients.
Diagnosis of Recurrent Urinary Tract Infections
Evaluation for recurrent UTIs goes beyond diagnosing a single infection. Doctors aim to understand patterns, triggers, and any underlying conditions contributing to repetition.
A thorough diagnostic workup may include:
Clinical Assessment
- Detailed medical history – Including frequency of infections, timing, potential triggers, bladder habits, sexual history, and prior treatments.
Laboratory Tests
- Urinalysis – Performed during active symptoms and sometimes afterward to confirm recovery.
- Urine culture and sensitivity – Done for each episode to identify specific bacteria and check antibiotic resistance.
- Post-treatment urine cultures – “Test-of-cure” to ensure the infection has fully cleared.
Imaging and Specialized Tests
Used when infections are frequent, severe, or unexplained.
- Renal and bladder ultrasound – Checks for kidney stones, tumors, or structural abnormalities.
- CT urography – More detailed imaging, used selectively.
- Voiding cystourethrogram (VCUG) – Evaluates vesicoureteral reflux in occasional cases.
- Intravenous pyelogram (IVP) – Rarely used today but may be considered in specific scenarios.
- Cystoscopy – Visual examination of the bladder and urethra to look for inflammation, stones, or structural problems.
Functional Evaluation
- Post-void residual urine measurement – Determines how well the bladder empties.
- Urodynamic studies – Assesses bladder pressures and voiding patterns.
- Vaginal examination – Especially in women with menopause-linked changes, pelvic organ prolapse, or vaginal atrophy.
Additional Screening
- STD testing – To rule out sexually transmitted infections.
- Diabetes screening – Fasting blood glucose and HbA1c.
- Immunodeficiency assessment – In patients with severe or unusually frequent infections.
This comprehensive evaluation helps tailor the best approach to both treatment and prevention.
Treatment of Recurrent Urinary Tract Infections
Treatment for recurrent UTIs has two parts: managing active infections and preventing future episodes. The exact plan depends on the severity, underlying cause, and patient preference.
- Treatment of Acute Episodes
During a flare-up, antibiotics remain the mainstay of treatment. The choice depends on urine culture results and resistance patterns.
Antibiotics commonly used include:
- Nitrofurantoin (5–7 days)
- Trimethoprim–sulfamethoxazole (3 days)
- Fosfomycin (single dose)
- Fluoroquinolones – Reserved for resistant infections
- Cephalosporins
Symptom relief may include:
- Phenazopyridine – A urinary analgesic to ease burning
- NSAIDs – To reduce pelvic pain or discomfort
- Preventive Strategies
Because prevention is key in recurrent UTIs, many patients benefit from long-term or targeted strategies.
Antibiotic Prophylaxis
Depending on individual risk, your doctor may recommend:
- Continuous low-dose antibiotics (6–12 months):
- Nitrofurantoin 50 mg at bedtime
- Trimethoprim–sulfamethoxazole (half tablet daily or 3 times weekly)
- Post-coital prophylaxis – A single antibiotic dose after sexual intercourse for UTIs triggered by sexual activity.
- Self-start therapy – A patient-initiated antibiotic dose at the very first symptoms.
- Antibiotic rotation – Cycling medications to reduce resistance.
Non-Antibiotic Prevention
For many individuals, non-antibiotic measures significantly reduce recurrence:
- Vaginal estrogen therapy – For postmenopausal women (cream, tablet, or ring)
- Cranberry products – Tablets or juice containing 36 mg proanthocyanidins daily
- D-mannose supplementation – 2 grams daily
- Probiotics (Lactobacillus strains) – Oral or vaginal
- Methenamine hippurate – A urinary antiseptic taken twice daily (1 gram per dose)
- Immunoactive prophylaxis – Using bacterial lysates
Lifestyle and Behavioral Measures
Daily habits can make a meaningful difference in preventing UTIs:
- Increased fluid intake – 6-8 glasses of water daily
- Regular and complete bladder emptying; don’t delay urination
- Double voiding technique – Urinate twice to ensure complete emptying
- Post-coital voiding – Urinate within 15 minutes after intercourse
- Maintain good hygiene:
- Wipe front to back
- Avoid douches and feminine sprays
- Change sanitary products frequently
- Cotton underwear – avoid tight-fitting synthetic clothing
- Avoid bladder irritants – caffeine, alcohol, spicy foods, artificial sweeteners
- Maintain regular bowel habits – prevent constipation
Treating Underlying Causes
In some cases, recurrent UTIs are linked to medical or anatomical issues that need specific treatment:
- Correcting anatomical abnormalities through surgery if needed
- Managing vaginal atrophy with estrogen therapy
- Manage diabetes and optimize blood sugar control
- Addressing pelvic organ prolapse with a pessary or surgical repair
- Managing urinary catheters or replacing them promptly (if catheter-associated)
- Treating stones in the kidney or bladder (lithotripsy or surgical removal)
Surgical Interventions (In Select Cases)
Surgery is not commonly needed but may be appropriate for certain structural or functional problems:
- Urethral dilation for strictures
- Transurethral resection for urethral diverticula
- Correction of vesicoureteral reflux
- Removal of foreign bodies or stones
Patient Education and Follow-up
Long-term success depends on empowering patients to recognize early signs and reduce triggers.
This may include:
- Keeping a symptom diary. Track triggers, patterns, and symptoms
- Regular follow-up appointments every 3–6 months
- Learning to identify early symptoms and respond quickly
- Addressing emotional stress or anxiety related to recurrent infections
- A multidisciplinary approach; including urologists, gynecologists, and infectious disease specialists, when needed
