Overview
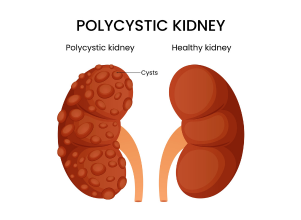
Polycystic kidney disease (PKD) is a genetic disorder in which numerous fluid-filled sacs, or cysts, develop in the kidneys. These cysts can enlarge the kidneys, reduce their function over time, and eventually lead to kidney failure in some cases.
PKD can occur in two main forms:
- Autosomal dominant PKD (ADPKD): The more common type, often developing in adulthood.
- Autosomal recessive PKD (ARPKD): A rarer type that usually appears in infancy or early childhood.
The disease progresses differently in each individual, with some experiencing mild symptoms for years and others developing significant complications early on.
Symptoms
Many people with PKD do not show symptoms in the early stages. When symptoms do occur, they may include:
- High blood pressure
- Back or side pain
- Enlarged abdomen due to kidney swelling
- Blood in the urine
- Kidney stones
- Frequent urinary tract infections
- Fatigue
- Headaches (often related to high blood pressure)
Severe cases may lead to kidney failure, requiring dialysis or a kidney transplant.
When to See a Doctor
If you have a family history of PKD or notice symptoms like persistent back pain, blood in the urine, or high blood pressure, consult a healthcare professional. Early diagnosis allows for better management and slows disease progression.
Causes
PKD is primarily caused by genetic mutations that affect the growth and development of kidney cells:
- Autosomal dominant PKD (ADPKD): A single copy of the mutated gene inherited from one parent can cause the disease.
- Autosomal recessive PKD (ARPKD): Requires two copies of the mutated gene, one from each parent, to manifest the disease.
The cysts in PKD continue to grow over time, gradually interfering with normal kidney function.
Risk Factors
The main risk factor for PKD is a family history of the disease. Other considerations include:
- Inheriting a defective PKD gene
- Age: Symptoms of ADPKD often appear between 30–50 years
- High blood pressure, which can worsen kidney damage
Diagnosis
PKD is often suspected if there is a family history or if a person shows symptoms such as high blood pressure, abdominal swelling, or kidney pain. Diagnosis usually involves a combination of the following:
- Imaging tests: Ultrasound, CT scan, or MRI can detect kidney cysts and monitor their growth over time.
- Genetic testing: Can identify mutations in the PKD genes, especially useful in families with a history of the disease.
- Urine tests: Check for blood or protein in the urine, which may indicate kidney damage.
- Blood tests: Assess kidney function by measuring levels of creatinine and blood urea nitrogen (BUN).
Early diagnosis is crucial, as it allows for monitoring kidney function, controlling blood pressure, and managing complications before significant kidney damage occurs.
Treatment
While there is no cure for PKD, treatment focuses on managing symptoms, slowing disease progression, and preventing complications. Approaches include:
- Blood pressure control: Medications such as ACE inhibitors or angiotensin receptor blockers (ARBs) help protect kidney function.
- Pain management: Over-the-counter pain relievers or prescription medications for chronic pain due to enlarged kidneys or cysts.
- Treatment of infections: Prompt use of antibiotics for urinary tract infections or kidney infections.
- Lifestyle modifications: Maintaining a balanced diet low in salt, staying hydrated, exercising regularly, and avoiding smoking and excessive alcohol.
- Cyst management: In some cases, large or painful cysts may be drained or surgically removed.
- Dialysis or kidney transplant: For patients whose kidney function declines significantly, renal replacement therapy may be necessary.
- Newer therapies: Certain medications may slow cyst growth and preserve kidney function in selected patients; these are prescribed and monitored by a nephrologist.
Regular follow-ups with a nephrologist are essential for monitoring kidney function, managing complications, and optimizing quality of life.
Complications
PKD can cause several complications if not monitored and managed:
- Kidney failure requiring dialysis or transplantation
- High blood pressure, which can increase the risk of heart disease
- Kidney infections or urinary tract infections
- Blood in the urine due to cyst rupture
- Liver cysts, pancreatic cysts, or aneurysms in the brain (in some cases)
- Chronic pain in the back, sides, or abdomen
Prevention and Management
While PKD cannot be cured, careful management can slow its progression and reduce complications:
- Regular monitoring of kidney function through imaging and lab tests
- Controlling blood pressure with lifestyle measures and medications
- Maintaining a healthy diet low in salt and rich in fruits, vegetables, and lean proteins
- Staying hydrated
- Avoiding smoking and limiting alcohol intake
- Prompt treatment of urinary tract infections and kidney stones
- Genetic counseling for individuals with a family history of PKD
Early diagnosis and consistent care can help people with PKD maintain kidney function for longer and lead a healthy, active life.
